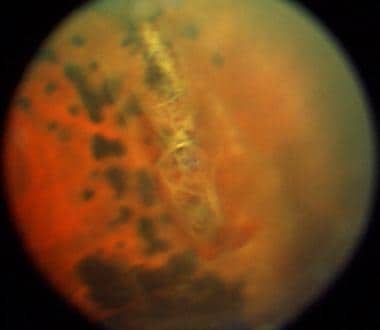
OCT imaging was also used to differentiate lamellar hole–associated epiretinal proliferation from classic or typical epiretinal membrane. The cavitated appearance was defined by the presence of a homogeneous round-edged hyporeflective space in the neurosensory retina. The schitic appearance was defined by the presence of multiple, narrow hyperreflective tissue bridges crossing wider hyporeflective spaces, located between the outer plexiform and outer nuclear retinal layers. In eyes with lamellar macular hole, lamellar separation of neurosensory retina demonstrated either a ‘‘cavitated’’ or a ‘‘schitic’’ appearance. Epiretinal membrane in a patient with macular pseudoholeĪnatomic OCT-based features of lamellar macular hole include the following: (1) an irregular foveal contour (2) a defect in the inner fovea (may not have actual loss of tissue) (3) intraretinal splitting (schisis), typically between the outer plexiform and outer nuclear layers and (4) features of photoreceptor layer. Thompson has no disclosures relevant to his talk.Figure 7. Thompson delivered at the Retina Subspecialty Day held prior to the 2017 American Academy of Ophthalmology meeting. Thompson, MD E: This article was adapted from a presentation that Dr. “If they have poor continuity, they are less likely to benefit from surgery.” “The most helpful thing in predicting surgical outcome is the continuity of the ELM/ellipsoid layer,” Dr. Thompson said.Įyes with prominent ERM may require surgery because they tend to have less favorable results if they are not treated. “Visual acuity, especially if it’s decreasing, should be the primary determinant of whether or not to offer surgery,” Dr. Most lamellar holes do not require treatment. Macular pseudoholes are a biomicroscopy diagnosis, and there may or may not be a lamellar hole.” “The central fovea may be thick, normal, or thin. “Almost all are associated with epiretinal membrane (ERM),” he added. “They are characterized as having an abnormally steep foveal contour. “Spectral-domain OCT is required to diagnose lamellar macular holes,” Dr. Thompson detailed additional differences between lamellar macular holes and macular pseudoholes. The study will share the results from patients at both 3 months and 1 year. Thompson has a study pending publication that includes 64 eyes with lamellar macular holes in patients with decreasing visual acuity. These same patients often have chronic diabetic macular edema or cystoid macular edema and they don’t tend to benefit from vitrectomy.Īlthough studies of surgical results for the treatment of lamellar macular holes have been positive, the studies tend to be small and are not randomized, Dr. Thompson also described a subgroup of patients who have secondary lamellar macular holes. The natural history of lamellar macular holes is reasonably good, and they don’t tend to progress.” Secondary holesĭr. Epiretinal membranes are virtually always present, and some eyes have lamellar hole-associated epiretinal proliferation. “I’d propose that there is often a steep irregular contour,” Dr. 
In contrast, a lamellar macular hole is defined by the appearance of the fovea via OCT. “Use pseudomacular holes only to describe the biomicroscopic appearance,” he added. Thompson defined pseudomacular holes as a clinical diagnosis as seen via slit lamp biomicroscopy versus optical coherence tomography (OCT). “One may fit the definition of a lamellar macular hole and the other a pseudomacular hole.”ĭr. “You can have two patients with similar central macular thickness,” Dr. So, are they fundamentally different disease entities? The central macular thicknesses are virtually identical (213 microns versus 208 microns). The patient at the top fits the definition of a lamellar macular hole while the patient at the bottom has biomicroscopic evidence of a pseudomacular hole.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
